If you’re wondering how dental implants work, you’re looking for a straightforward explanation. Dental implants replace missing teeth through a surgical process where a metal post is implanted into the jawbone and topped with a realistic dental crown. This guide will explain the simple yet sophisticated technology behind dental implants, the procedural steps from consultation to full recovery, and what benefits dental implants offer for your oral health and daily comfort.
Key Takeaways
- Dental implants are a permanent and natural-feeling solution for missing teeth, anchoring artificial teeth to jawbones through titanium posts to prevent common issues associated with traditional prostheses.
- The dental implant process is meticulous and can take several months to over a year, involving removal of damaged teeth, jaw preparation, and various surgeries, highlighting the need for patient commitment and prudent financial planning.
- Maintaining dental implants involves meticulous oral hygiene practices, avoiding hard foods and smoking, regular dental checkups, and careful monitoring to ensure their longevity and functionality.
Demystifying Dental Implants: A Modern Solution for Missing Teeth
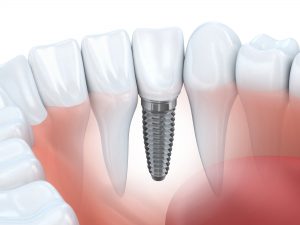
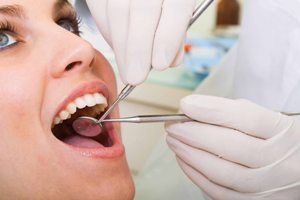
Dental implants are game-changers in the field of dentistry. If you’re considering dental implants in Rockville, these artificial teeth are attached to titanium posts anchored to the jawbone, providing a sturdy and reliable solution for missing teeth. They offer a natural feel and appearance, closely resembling your real teeth. Additionally, dental implants prevent bone damage and other common issues associated with dental prostheses, such as slippage and noise.
Fully appreciating the benefits of dental implants requires a grasp of their intricate details. This type of dental surgery, performed by oral and maxillofacial surgeons, offers a sturdy foundation for new teeth, which is vital for activities such as eating and speaking. Dental implants interact seamlessly with your natural teeth, safeguarding your oral health and greatly improving your dental comfort. Some key benefits of dental implants include:
- Sturdy foundation for new teeth
- Improved ability to eat and speak
- Seamless interaction with natural teeth
- Safeguarding of oral health
- Enhanced dental comfort
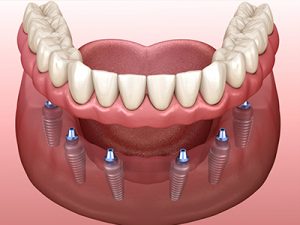
Understanding the Components of a Dental Implant
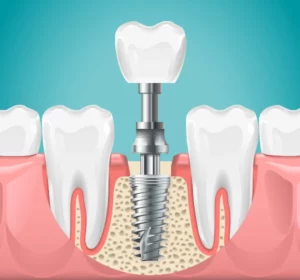
A dental implant is a sophisticated assembly of a titanium or ceramic screw, an abutment connector, and a dental crown. The screw, or the implant, is surgically placed into the jawbone and serves as the root structure for the artificial tooth. Attached to the titanium post is the abutment, a connector piece that extends above the gum line to provide a base for the dental crown.
The components of a dental implant include:
- The implant, which is surgically placed into the jawbone
- The abutment, which connects the implant to the crown
- The crown, or the artificial tooth, which visually and functionally replaces the missing tooth
This complete structure forms a dental implant, providing a firm and natural-looking replacement tooth.
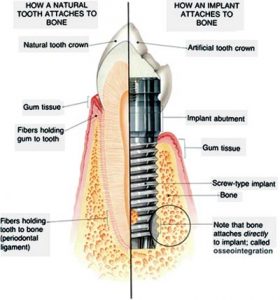
The Role of Osseointegration in Dental Implants
A critical aspect of dental implants is osseointegration, a process where the jawbone grows around the dental implant, providing it with the necessary strength and stability. During osseointegration, the jawbone integrates with the surface of the dental implant, a process that may involve additional steps like bone grafting and can typically take 4-6 months to complete.
The successful fusion of the jawbone with the dental implant, known as osseointegration, hinges on bone quality, gum health, and diligent oral hygiene to ward off infections.
The Journey to Getting Dental Implants: What to Expect
The journey to getting dental implants is a comprehensive process, requiring commitment and patience. It typically involves the following steps:
- Removal of damaged teeth
- Preparation of the jawbone
- Placement of the metal implant post through drilling into the jawbone
- Healing period for bone growth
- Abutment placement
- Attachment of the artificial tooth
This procedure requires a multidisciplinary approach, with an oral and maxillofacial surgeon, also known as an oral surgeon, for implant placement, and a prosthodontist for prosthetic work, supported by a team of dental technicians who craft the prosthesis with precision. Oral and maxillofacial surgery plays a crucial role in ensuring the success of this procedure.
The timeline for dental implant treatment varies, often extending from two months to over a year. This prolonged process, which may include extractions or bone grafting, demands patient dedication. Preparation involves pre-surgical steps such as taking impressions and adhering to a soft food diet after surgery. Patients should also be ready for a healing period before the placement of permanent crowns, which usually involves several follow-up appointments. It’s also important to evaluate insurance and payment options when deciding to proceed with dental implants, highlighting the need for prudent financial planning.
Initial Assessment: Are You a Good Candidate for Dental Implants?
The initial assessment for dental implants involves a comprehensive dental exam that includes a health history review and X-rays to measure bone density and determine the suitability of the bone for implant placement. Key eligibility criteria for dental implants include good general oral health, absence of oral infections, a fully developed and healthy jawbone, and healthy gums.
Certain individuals, such as pregnant women, those with chronic diseases or immunosuppression, and those who exhibit significant teeth grinding, may not be good candidates for dental implants. A dental hygienist typically evaluates patients to determine their candidacy during the consultation process.
Surgical Insight: The Dental Implant Placement Process
The dental implant placement process, also known as the dental implant procedure, is a surgical procedure that requires precision and expertise. During the surgery, the following steps are taken:
- A cut is made in the gums to access the jawbone.
- Holes are drilled in the jawbone to accommodate the implant post.
- The implant post is then implanted deep into the bone.
This procedure is typically performed under local anesthesia or sedation, ensuring that patients do not experience pain during the surgery.
The abutment, which serves as the connection piece for the crown, may be attached to the implant during the initial surgery or in a subsequent procedure after the jawbone has integrated with the implant. The entire procedure for placing a single dental implant typically lasts only one hour, with most patients finding over-the-counter pain relievers sufficient for managing post-procedure discomfort.
Life After Dental Implants: Recovery and Care
Life after dental implants involves a recovery and care process to ensure the longevity and functionality of your new teeth. Post-surgical discomfort can often be managed with over-the-counter pain relievers like ibuprofen, and for more severe pain, prescription medication may be prescribed. To reduce post-surgical swelling, ice can be applied intermittently to the affected area during the first 24 hours.
Patients should also practice proper oral hygiene with gentle cleaning around the implant using a Q-tip after a few days. Rinsing with a warm saltwater solution several times a day is recommended starting after the first day of surgery, especially after eating, to support healing.
Patients should follow these guidelines after dental implant surgery:
- Avoid strenuous activity for a few days
- Abstain from smoking for at least two weeks
- Return to a normal diet after 3-4 days, but avoid biting on hard items near the implant site and avoid hot liquids and spicy items for a few days
- Avoid excessive pressure on the implant site to prevent implant failure
- Consider using a dental appliance like a bite guard if you have bruxism or if you are a smoker
Following these guidelines will help facilitate the healing process and ensure the success of your dental implant.
Regular dental checkups are essential for monitoring the health of dental implants and ensuring their longevity and functionality.
Navigating the Healing Process: Tips for a Smooth Recovery
The healing process following dental implant surgery calls for diligent care and patience. Patients often experience discomfort such as:
- swelling
- bruising
- pain
- minor bleeding at the implant site
Practicing good oral hygiene right after the surgery is paramount for proper healing and the longevity of the implant.
Recovery may involve follow-up appointments for procedures such as the placement of a healing cap during an ‘uncovery’ appointment, and for the removal of stitches if they are not self-dissolving. Early detection and management of inflammatory processes around dental implants are essential to improve the long-term prognosis of the treatment.
Maintaining Your New Artificial Tooth: Long-Term Care Strategies
Adopting and maintaining long-term care strategies are key to ensuring the success and longevity of your dental implants. These strategies include:
- Meticulous oral hygiene practices such as brushing and flossing after each meal
- Rinsing with an antiseptic mouthwash
- Steering clear of sugary or acidic drinks
- Regular dental checkups and professional cleanings
These practices are vital for monitoring and maintaining the health of your dental implants.
Moreover, it’s important to avoid chewing in the area of the implant and abstain from hard foods to prevent trauma, ensuring the health and functionality of the implant. Adherence to a consistent homecare routine is essential to prevent peri-implantitis and ensure the long-term success of dental implants.
Enhancing Oral Functionality: The Benefits of Choosing Dental Implants
Dental implants contribute significantly to enhancing oral functionality. They offer numerous aesthetic and functional benefits, including:
- Restoring a person’s confidence and well-being, allowing them to smile, talk, eat, and live more confidently
- Preventing bone loss by preserving the natural shape of the jawbone
- Providing a stable base for replacement teeth
- Improving appearance and adding support for surrounding tissues
Overall, dental implants play a crucial role in improving oral health and overall quality of life, as dental implants work effectively in replacing missing teeth.
Compared to dentures or bridges, dental implants provide:
- Greater stability and bite force, allowing for easier consumption of different types of food
- Improved overall chewing experience
- More natural ability to eat and speak when compared to traditional dentures, eliminating the worry about denture fit or the need for adhesives
Flexible options for artificial teeth include both removable and fixed prosthetics, catering to the specific needs and preferences of the patient post dental implant surgery. Dental implants offer a more natural ability to eat and speak when compared to traditional dentures, eliminating the worry about denture fit or the need for adhesives.
How Dental Implants Can Restore Chewing Ability and Speech
Dental implants play a key role in restoring chewing ability and speech. Firmly anchored in the jawbone, they provide a stable base for artificial teeth, leading to enhanced biting and chewing capabilities. The stability of dental implants helps prevent the slippage or instability common with dentures, thus improving the chewing process. Unlike dentures or bridges that can slip and cause awkward chewing, dental implants bring biting and chewing functions close to pre-tooth loss conditions.
Furthermore, dental implants can improve speech by:
- Preventing the movement of teeth that can occur with dentures, allowing for clearer and more confident speech
- Filling in gaps with dental implants that function similarly to natural teeth, so patients can articulate words more precisely
- Avoiding the mumbled or slurred speech sometimes associated with missing teeth or poorly fitting dentures.
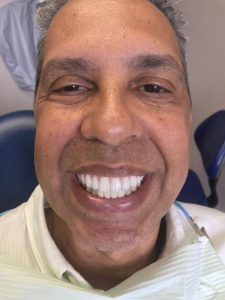
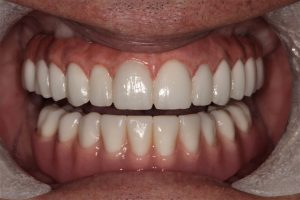
The Esthetic Appeal: Dental Implants and the Natural Shape of Your Smile
Beyond functionality, dental implants offer several esthetic benefits, including:
- They are designed to look and feel like natural teeth, providing a seamless addition to a patient’s existing smile.
- The structure and stability of dental implants help to maintain the natural shape of the mouth.
- Dental implants prevent bone loss, preserving the facial contours.
With dental implants, a restored and aesthetically appealing smile can enhance social interactions and open up new professional opportunities.
Advanced Considerations: When Additional Procedures are Necessary
In some cases, additional procedures might be necessary for successful implant placement. For instance, bone grafting is required when the jawbone isn’t thick enough or is too soft to support an implant. The purpose of a bone graft is to create a solid base for the dental implant, ensuring stability and a reliable foundation for the new teeth.
After bone grafting, it can take several months for the bone to grow enough new tissue to support a dental implant, with the healing period potentially extending up to approximately four months. These materials for bone grafts can be natural bone from the patient’s own body or synthetic alternatives, depending on the specific needs of the case.
The Necessity of Bone Grafts for Successful Implant Placement
Bone grafting is often required when the jawbone is not thick enough or is too soft, which is necessary to provide the support needed for dental implants. The bone grafting procedure involves adding natural or synthetic bone graft material to areas of the jawbone deficient in bone mass to ensure a solid foundation for implants.
Part of the dental implant treatment plan includes taking X-rays to determine if there is adequate bone in the upper and lower jaws and to establish whether a bone graft might be required.
Managing Gum Tissue Health in Preparation for Implants
Before implant surgery, it’s imperative to manage gum tissue health. The success of dental implants hinges on healthy oral tissues, and those with compromised gum health may not be suitable candidates for the procedure. Prior to dental implant surgery, it’s necessary to evaluate a patient’s risk factors for gum disease to ensure a favorable outcome. Stabilizing any existing oral disease before implant placement is vital in warding off implant-related diseases and potential failure.
Prior to implant surgery, the patient’s gums must be in optimal condition and free from disease to diminish the risk of post-surgical infection.
Summary
In conclusion, dental implants offer a comprehensive solution for missing teeth, enhancing oral functionality, and boosting self-confidence. From understanding the components of dental implants and the role of osseointegration to navigating the journey of getting dental implants and life after, it’s evident that dental implants have revolutionized dental treatment. They provide an aesthetically appealing and functional alternative to traditional dentures and bridges. However, it’s essential to understand that successful dental implant treatment requires commitment and careful consideration of various factors, including oral health, bone density, and potential need for additional procedures.
Frequently Asked Questions
Is it painful to have dental implants put in?
Getting dental implants can involve some discomfort, typically ranging from a pain level of two to three in the first 24 to 48 hours, which can be managed with over-the-counter medication like Tylenol or Advil.
How are dental implants done step by step?
Dental implants are done in several steps, including damaged tooth removal, jawbone preparation, dental implant placement, bone growth and healing, abutment placement, and artificial tooth placement.
What are the 3 stages of dental implants?
The three stages of dental implants are the placement of the implant into the jawbone, followed by the addition of the abutment, and finally the placement of the prosthetic tooth or crown.
How long does a dental implant last?
In general, a dental implant can last a lifetime with proper care, while the crown may need replacement after 10 to 25 years due to wear and tear. Regular dental check-ups can help ensure the longevity of the implant.
What are the components of a dental implant?
A dental implant consists of a titanium or ceramic screw, an abutment connector, and a dental crown. The screw serves as the root structure, the abutment provides a base, and the crown visually and functionally replaces the missing tooth.